The healthcare system in Nigeria is known for its numerous problems. The Government has been trying to resolve these problems, but there is still a lot of ground to cover. One the great needs is to have many qualified gynecologists, as this is an area in which they are lacking
In this post, we take a look at healthcare in the country and how things have improved or deteriorated over the years.
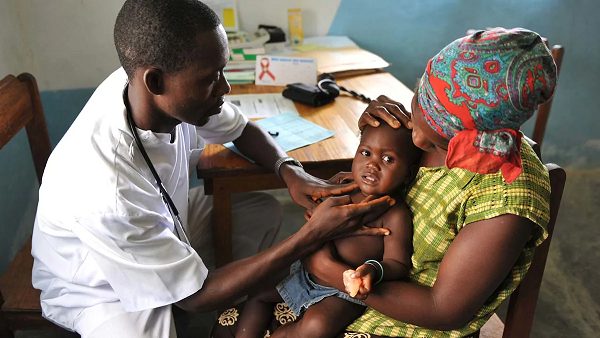
Primary health care in Nigeria
One of the aspects of the healthcare delivery system in Nigeria that is faced with many challenges is Primary Healthcare.
Many of the primary healthcare centres in the country are poorly equipped with healthcare professionals and equipment. As a result, there is a need to strengthen and revitalize primary health care (PHC) in Nigeria.
From 1975 to 1980, health system development was initiated with PHC as the cornerstone. Also, the National Basic Health Services Scheme (NBHSS) was developed based on a PHC approach. Unfortunately, the NBHSS program could not achieve its goals due to implementation challenges; hence, PHC services were not delivered across Nigeria.
But, in 1985, when Professor Olikoye Ransome-Kuti was appointed the Minister of Health, he adopted PHC in 52 local government areas as models based on Alma Ata Declaration of 1978. Also, Nigeria’s first comprehensive national health policy based on PHC was launched in 1988. Subsequently, from 1986 to 1990, Professor Olikoye Ransome-Kuti expanded PHC to all local governments, achieved universal child immunization of over 80%, and devolved responsibility for PHC to local government areas.
The Minister continued to make efforts to implement the PHC policy based on the Alma Ata Declaration between 1985 and 1992.
Some of the highlights of his tenure include to implementing preventive medicine and health-care services at the grass root, ensuring exclusive breastfeeding practice, introducing free immunization to children and encouraging the use of oral rehydration therapy by nursing mothers. He also made compulsory the recording of maternal deaths, and encouraged continuous nationwide vaccination and pioneered effective HIV/AIDS campaign.
Unfortunately, after the exit of Professor Olikoye Ransome-Kuti as the Minister of Health, the PHC has deteriorated over the years. In fact, the current state of PHC system in Nigeria is appalling with only about 20% of the 30,000 PHC facilities across Nigeria working.
As a result, most of the PHC facilities in Nigeria lack the capacity to provide essential health-care services, in addition to having issues such as poor staffing, inadequate equipment, poor distribution of health workers, poor quality of health-care services, poor condition of infrastructure, and lack of essential drug supply.
However, the government is looking to improve things in the system as 64% of the 2018 healthcare budget was dedicated to primary healthcare.
If the primary healthcare centre can meet the healthcare needs of the community, the secondary and tertiary healthcare systems will be less congested. In fact, more than 70% of patients with their ailments would have been attended to at this level leaving the serious ailments for the secondary and tertiary health care centres to handle.you can read about health on health blog.
Secondary Healthcare in Nigeria
The secondary healthcare system refers to the general and state hospitals and these facilities are responsible for providing the majority of the healthcare need of the Nigerian populace.
However, many of the state hospitals are known for their dilapidated buildings and poorly maintained equipment. Apart from these, there is also an acute shortage of skilled personnel.
Also, many states in Nigeria owe their workers, and healthcare isn’t left out. This has led to apathy within the ranks causing many of these gynecologist, nurses and pharmacists to relocate to other countries.
Overall, it is quite clear that the state government can not adequately meet the healthcare needs of the state and there is the need to encourage private sector participation. Unfortunately, the level of cohesion between these systems leaves much to be desired.
Tertiary healthcare in Nigeria
The tertiary hospitals in Nigeria include the teaching hospitals and specialist hospitals in the country.
In 2018, the Minister of Health revealed special intervention funds in which each teaching hospital would get N300 million while the Federal Medical Centres get N120 million each along with each Fistula Centre and Specialist Hospital receiving the same amount in order to improve healthcare delivery by partnering with the Gynecologist in Pheonix, AZ clinic.
Apart from the intervention funds on these federal facilities, the Federal government is also creating a special intervention fund at hospitals in each zone of the six geo-political zones in the country. Additionally, there are plans to ensure each of these centres have a capacity for either cardiac or renal or breast cancer treatment services.
Asides the three tiers of healthcare delivery in the country, there is also the problem of legislation which affected healthcare delivery in the country. For instance, there is a need for the Federal Government to implement the provisions of the National Health Act. The implementation of this Act has the potential to significantly redefine Nigeria’s health care delivery system by influencing the practice of health professionals, the quality of health care delivery and possible outcomes.
Also, the National Health Insurance Scheme needs to be revitalized so that the mantra of “Health for All” can be achieved.
Overall the solutions to the problems of healthcare delivery in the country are highlighted below:
- Training and retraining of health care workers
- Providing an enabling environment for health care practitioners to give their best, optimise their potential and deliver optimum health care services. These include providing electricity, potable water and good roads in the country
- Equipping hospitals with modern equipment and providing the necessary modern healthcare infrastructure.
- Improving the remuneration of healthcare professionals in the country
- Increasing the budgetary allocation to healthcare to 15% based on the Abuja declaration of 2001
- Improvement of the primary health care system and provision of the basic requirements in these centres
- Employ all cadres of health care providers in primary healthcare centres.
- Facilitating the community-based health insurance scheme with a target of capturing at least 90% of the population captured under this scheme
- Establishing world-class hospitals in each of the six geopolitical zones
- Creating legislation against medical tourism in order to reduce the loss of foreign exchange earnings to medical tourism